Targeting Phase 1 commissioning by the end of 2026
HIGHLIGHTS
-
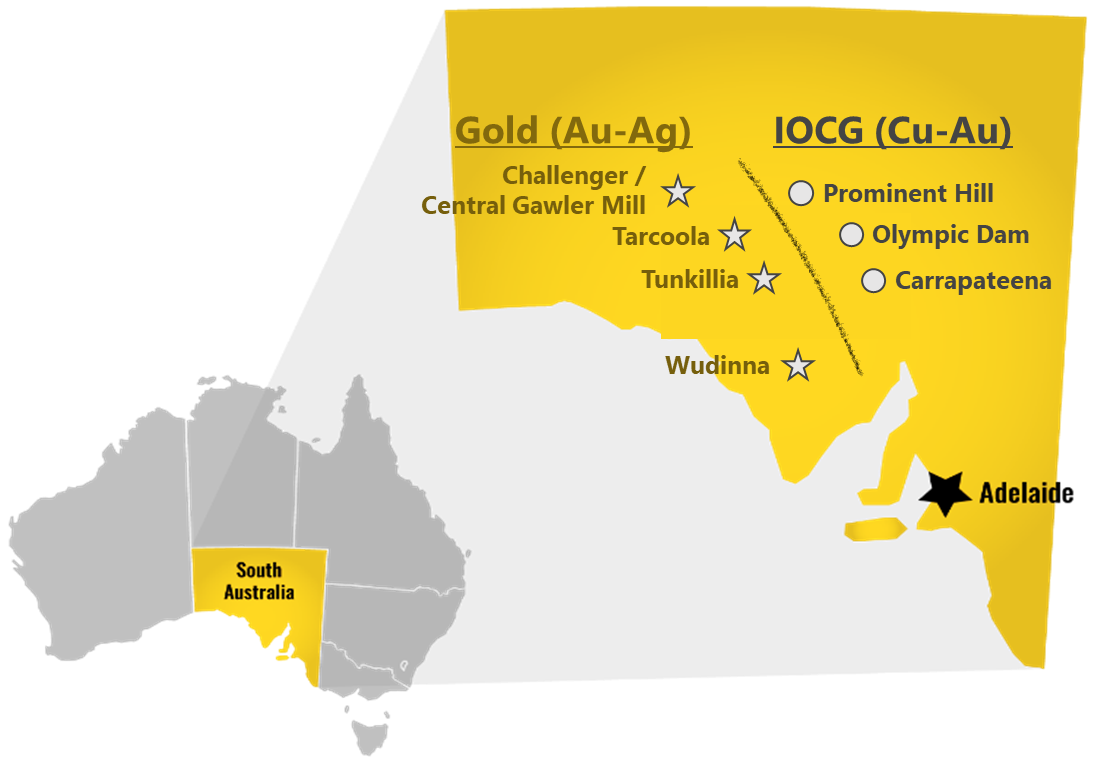
Existing fully permitted Central Gawler Mill adjacent to brownfield Challenger mines
-
Challenger JORC (2012) Mineral Resources Estimate now 313koz Au (10.6Mt @ 0.92 g/t), including 194koz Au (1.87Mt @ 3.23